Pinched Nerve Relief
But Is It Really a Pinched Nerve? How To Overcome One of the Most Commonly Misnamed Conditions
Robert Inesta
2/12/20258 min read

A term that’s commonly used (often incorrectly) is the "pinched nerve." This term is often used in both clinical settings and everyday language, but is frequently misunderstood. In this article we will explore what exactly is a pinched nerve, the physiological and anatomical mechanisms involved, common misconceptions, and what you can do about it.
As a chiropractor, acupuncturist, and myofascial manipulation practitioner, I believe it’s essential to educate both patients and the general public on common neuromusculoskeletal conditions, clear up misunderstandings and provide practical actionable solutions. Understanding the causes and mechanisms of common conditions can empower people to take control of their bodies, heal faster and prevent recurrences.
What Exactly is a Pinched Nerve?
A pinched nerve, technically known as neural compression, nerve entrapment, or nerve impingement, is a type of peripheral neuropathy that occurs when surrounding tissues exert excessive pressure on a nerve or nerve root. This excessive pressure is the so called “pinch”. This can happen for a variety of reasons, including but not limited to herniated or bulging discs, tight muscles and fascia, scar tissue, bone spurs, arthritis, or other injuries. The resulting compression causes irritation that affects the ability the nerve to transmit signals and can cause symptoms such as pain, numbness, tingling sensations and even weakness in the muscles innervated by the affected nerve.
To fully understand the phenomenon of a pinched nerve, let’s explore the anatomy of a nerve. Here we are specifically talking about peripheral nerves that extend from the spinal column. These nerves carry signals between the brain, spinal cord, and the rest of the body. They relay both sensory (feeling ad positional) information and motor (muscle) function commands.
Nerve roots emerge from the spinal column and extend outward forming nerves that go to different parts of the body running through and between muscles, fascia, tendons, ligaments, and bones.
Nerves are composed of bundles of individual nerve cells (neurons) consisting of fibers called axons that carry electrical impulses. Each nerve is encased in a protective sheath of connective tissue as a whole, which provides structural support and protection. Interestingly, each nerve fiber is encased in a thin layer of this connective tissue, and groups of nerve fibers called fascicles are wrapped in another layer. These fascicles all encased together is what forms the nerve.
Many nerve fibers are insulated by a myelin sheath made of fatty substance. This sheath enhances the speed of signal and impulse conduction.
Nerves also have a blood supply that brings nutrients and oxygen to the neurons and carries away metabolic waste products.
Function of Nerves
The primary function of nerves is communication within the body. This can be broken down further to:
Signal Transmission: Nerves facilitate communication between the brain, spinal cord, and the rest of the body, allowing for sensory perception, motor (muscle) function, and autonomic regulation (involuntary organ function).
Response Coordination: Nerves coordinate responses to stimuli by exchanging information between sensory receptors, the brain, and effectors (muscles or glands).
Reflex Actions: Nerves are involved in reflex arcs that enable rapid responses to stimuli without direct involvement of the brain.
Physiological Mechanism of Nerve Compression
Neural compression or impingement occurs when another tissue exerts pressure on a nerve, which can cause irritation and lead to pain and disruption of function. The following physiological mechanisms are involved:
Reduced Blood Flow: Compression can diminish blood supply to the nerve, leading to ischemia and insufficient oxygen and nutrients. This can result in dysfunction.
Axonal Deformation: Compression can cause physical deformation of the nerve fibers, impeding the transmission of electrical impulses. This may lead to altered sensations, pain, or muscle weakness.
Chemical Changes and Inflammatory Response: Compression can elicit an inflammatory response, leading to swelling of surrounding tissues. This further exacerbates nerve compression, creating a cycle of worsening symptoms. While inflammation is actually a necessary aspect of the healing process, if it is uncontrolled and becomes chronic, it is problematic. The release of inflammatory mediators (e.g., cytokines and prostaglandins) from injured or irritated tissues can sensitize the nerve, heightening pain responses even to non-painful stimuli (a phenomenon known as allodynia).
Demyelination: In some cases, sustained compression can damage the myelin sheath, resulting in slowed or disrupted signal transmission, which can cause long-term functional impairments.
Symptoms of a Pinched Nerve
The symptoms of a pinched nerve are diverse and may include one or any combination of the following:
Localized Pain: Sharp or aching pain in the affected area.
Radiating Pain: Pain that travels along the nerve pathway, which can manifest in different regions of the body depending on which nerve is affected.
Numbness: Loss of sensation in the area the nerve innervates
Paresthesia: Altered sensations such as tingling, pricking or burning.
Weakness: Reduced strength in the muscles controlled by the affected nerve.
The manifestation of symptoms largely depends on the location of the pinched nerve and the significance and type of compression.
Some examples of common conditions that can be considered “pinched nerves” are:
Sciatica
Carpal Tunel Syndrome
Cervical Radiculopathy
Lumbar Radiculopathy
Ulnar Neuropathy
Radial Nerve Entrapment
Thoracic Outlet Syndrome
Common Causes of a Pinched Nerve
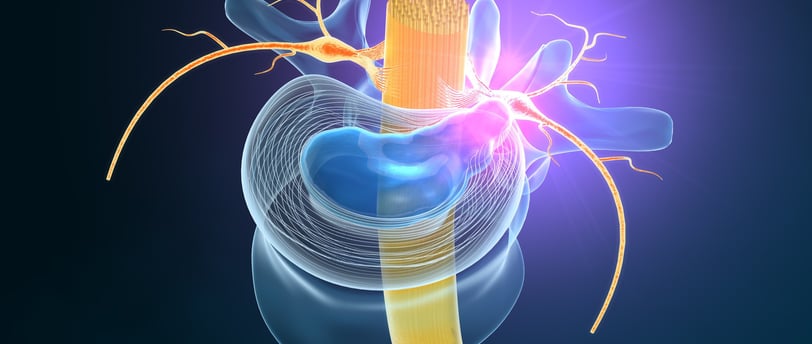
Herniated Disc or Bulging Disc: One of the most common causes of a pinched nerve occurs when a lumbar or cervical disc herniates or bulges. When the soft inner material of the disc bulges out, it can impinge on the exiting nerve roots. Sometimes just the inflammation caused by the bulged or herniated disc material can chemically irritate the nerve root even if not being physically compressed.
Bone Spurs: Age-related changes can lead to the development of bone spurs, which can further narrow spinal canals and compress nearby nerves.
Arthritis: Conditions such as osteoarthritis can cause the joints to become inflamed and lead to a narrowing of the spaces around the nerves.
Traumatic Injuries: Impact trauma can cause direct crush injuries to nerves. Soft tissue injuries or fractures can alter the alignment of bones and cause swelling and scarring resulting in nerve compression.
Repetitive Movements: Certain occupations, sports, or activities that require repetitive motions may lead to muscle and fascial tension and distortions that eventually cause or contribute to pinched nerves.
Posture and Body Mechanics: Poor ergonomics and posture can create tension points in muscles and fascia and eventually degeneration and distortion in joints that can impinge and irritate nerves.
Muscle Tightness: When muscles become tight or go into spasm, they can compress nearby nerves. This is particularly common in areas where nerve pathways run through or in between muscles, such as the scalene muscles of the neck, subscapularis and pec minor of the shoulder and piriformis and hip external rotator muscles.
Fascial Adhesions: The connective tissue (fascia) can develop adhesions or scar tissue formation due to repetitive tension, injury or surgical procedures. These adhesions can create distortions and restrictions that limit the free movement of adjacent nerves, making them more susceptible to compression and irritation.
Tumors: this is rare but important to mention. There are times when a mass or tumor can physically impinge a nerve causing common nerve symptoms. Masses can include cysts, benign tumors (non-cancerous) or malignant tumors (cancerous). These cases require immediate medical attention to determine the appropriate course of action.
Misconception About Pinched Nerves
“Pinched nerve” is one of the most commonly misused terms I’ve heard over the years in practice. Often, people who have a sharp localized pain in the neck or shoulder think it is a pinched nerve. I’ve even heard of doctors diagnosis patients with a pinched nerve in these situations which is clearly inaccurate.
While nerve entrapments can cause localized pain, most of these cases of local neck or shoulder pain are due to muscle, fascia or joint issues and do not have nerve involvement. Even disc injuries can cause intense local pain without having nerve involvement. Typically if there is actual nerve impingement or compression, nerve symptoms will be present such as numbness, tingling, pain along the nerve route, or weakness.
Diagnosis and Treatment
There is a lot you can do on your own to relieve and overcome a pinched nerve. It’s usually best to seek the help of a competent professional to properly evaluate, diagnose, and guide you in the best course of action. Every individual is different with different variables and needs. Chiropractors, osteopaths, orthopedists, neurologists, physical therapists and physiatrists are often the types of practitioners people will consult with for nerve impingement.
Evaluation should include a thorough history/consultation and physical exam. Diagnostic imaging such as x-ray and MRI may be warranted. In more stubborn or severe cases, electromyography/nerve conduction velocity testing could be warranted. This is a physiological test that can determine if there is functional change in the nerve and where the problem is located.
Once the problem is properly identified, targeted treatment can begin.
It’s best to address nerve issues as soon as possible. There are varying degrees of severity and concern, but if ignored, the condition may worsen and can lead to permanent nerve damage. Cases involving motor function loss (muscle weakness) or atrophy are more concerning and often need a more aggressive approach.
The majority of cases of nerve impingement can be treated successfully with natural approaches.
Some of the most effective natural options include:
Activity Modification: Modifying activities that exacerbate symptoms can help alleviate nerve irritation. This can include improving ergonomics of a workstation (altering monitor height, standing desks and changing mousing patterns), changing workout or training routines, being mindful of posture and repetitive movements.
Exercise/Movement Therapy: A physical therapist, chiropractor or good trainer can provide exercises and stretches designed to relieve pressure, strengthen supporting muscles, and mobilize the nerves, which can help restore function and reduce discomfort. “Nerve flossing” is a great example of an exercise to help restore movement to nerves and alleviate nerve entrapments and can be done on the major peripheral nerves in the arms and legs.
Myofascial/Soft Tissue Manipulation: Techniques such as Stecco Fascial Manipulation and Active Release Techniques (A.R.T.) can help release tension from the fascia and muscles, mobilize adhesions, and address distortions, allowing the nerve to move more freely without irritation.
Chiropractic: Chiropractic adjustments can help mobilize the spine and other joints, improving function and alleviating nerve irritation.
Acupuncture or Dry Needling: This involves inserting thin needles at specific points to relieve pain, regulate and calm the nervous system, release tension from the surrounding muscles and fascia, and improve microcirculation to the nerve.
Passive Therapies such as Heat, Infrared, Red Light, Laser, PEMF: Applying passive therapies can help resolve inflammation, improve blood flow and control pain.
Mindfulness and Stress Management: Techniques such as meditation, deep breathing exercises, and mindfulness can help manage pain perception and reduce stress, which can cause and amplify muscle tension and pain. Maintaining a healthy mindset and understanding the pain process is also important and helpful in healing.
Yoga, Tai Chi and Gentle Stretching Techniques: Gentle yoga and targeted stretching exercises can improve flexibility and strengthen supporting muscles.
Supplements and Herbal Remedies: Some herbs, such as turmeric (known for its anti-inflammatory properties) and ginger, may help reduce inflammation and pain. Omega 3 fatty acids can be helpful for nerve support and have anti-inflammatory properties. Always consult a healthcare professional before starting any herbal supplements.
Diet and Hydration: Maintaining a nutrient-rich, anti-inflammatory diet consisting of clean, organic whole foods, avoiding unnatural, processed inflammatory junk foods, and staying properly hydrated are important for all aspects of health but also help support the healing process.
Sleep: Sleep is essential for healing and recovery. It’s when the body does its major repair work. For the average adult, seven to eight hours of sleep is usually adequate. If dealing with an injury though, an eight hour minimum would be a better target.
I prefer a comprehensive approach combining the above for best and fastest results.
If a case is more severe and not responding to natural care, medical options would typically be oral medication, injections and in the worst cases surgery.
Conclusion
Nerve impingement or a “pinched nerve” as it’s commonly referred to, can range from mildly annoying to severe and debilitating but it doesn’t have to take over your life. It is usually more than just a localized pain in the neck or shoulder, typically involving neurological symptoms including numbness, tingling, pain along the course of the nerve, and in more severe cases muscle weakness.
There is much you can do both naturally and on your own to relieve pain and heal and overcome a pinched nerve. If you are suffering with this condition or with symptoms you think may be caused by nerve impingement, its always a good idea to seek the help of a professional who’s experienced in diagnosing and treating it appropriately.
As always, know that there’s hope and your body can and will heal if you give it what it needs. Start taking steps to give it the right support so it can heal in the most efficient manner.
Berkshire Functional Chiropractic & Acupuncture
Join Our community for education, resources, and updates
info@berkshirefunctional.com
(413) 274-7161
© 2024. All rights reserved.
